Venous diseases
Varicose veins are one of the most common diseases in Europe. According to recent research, every fifth woman and every sixth man shows signs of this disease. One in four people over 40 is already affected.
Common complaints are pain, swollen and heavy legs, as well as itching.
The most feared complications include phlebitis (superficial thrombosis), deep vein thrombosis (obstruction of the deep veins), skin lesions (increased or decreased pigmentation, eczema), and chronic wounds (leg ulcer, open leg).
The cause is predominantly a genetic predisposition. Pregnancy, physical inactivity, obesity, and standing or sitting may accelerate varicose veins and increase discomfort.
Various forms of varicose veins may occur singly or in combination
Spider veins and reticular varicose veins
These are very superficial venous plexuses. These are usually harmless, but often cosmetically disturbing.
Lateral varicose veins
Expanded and clearly visible veins on the upper or lower leg.
Stem vein weakness
This is usually not visible and only noticeable through effects such as sappethral veins or leg discomfort.
Diagnostics
Advances in medical technology make it possible to study varicose veins today without side effects and stress on the body. The previously performed contrast agent examinations only need to be performed in very rare cases.
We carry out the following examinations:
Digital Photoplethysmography (DPPG)
In this brief examination, the filling status in the superficial venous system is measured. Disorders of the function of the venous system on the leg can be detected.
Color-coded Ultrasound Examination (color duplex)
With the help of ultrasound, an exact representation of the superficial and deep vein system can be made. The function of the vessels is examined at the same time. Valve weakness in the deep or superficial venous system can usually be detected easily.
This examination is without side effects and can be repeated as often as desired. With the help of an ultrasound examination, the presence of an acute deep vein thrombosis can either be proven or excluded in most cases.
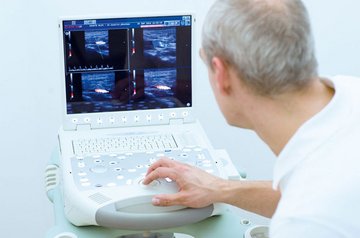
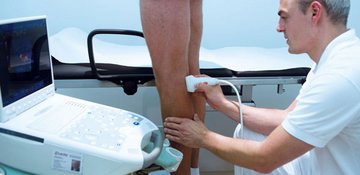 Examination of vascular functions with a color-coded ultrasound examination
Examination of vascular functions with a color-coded ultrasound examination
Treatment options
The following treatment options for varicose veins are possible, and are all performed in our clinic:
- Sclerotherapy including foam sclerotherapy
- Laser therapy of spider veins
- Phlebectomy (so-called crocheting method) of saphenous veins
- Classic crossectomy and stripping of the stem veins
- Radiofrequency therapy (VNUS Closure Fast) of the stem veins as an alternative to the crossectomy
Every person is different. Therefore, our goal is to give an individual treatment recommendation after a thorough examination.
Sclerotherapy including foam sclerotherapy
Injecting a drug (e.g.: Aethoxysklerol) into varicose or spider veins causes artificial inflammation of these vessels; the veins can then stick together, be dissolved and removed by the body. A further development of this method is the use of a so-called microfoam. This is an approved form of therapy in which the classic sclerosing agent is "foamed" by mixing it with a gas / air mixture. Many studies have shown a better efficacy of this method compared to classic sclerotherapy, with the same level of safety.
Phlebectomy (so-called crocheting method)
This procedure is a "mini-surgical procedure" for the removal of small or medium-sized varicose veins, using stitches of only a few millimeters in length and then pulling out the veins with a special instrument (crochet method) or severing them ideally without a visible scar.
Classic crossectomy and stripping of the stem veins
Still, this classic form of venous operation is considered by most venous specialists to be standard procedure in varicose vein treatment. A small incision in the groin (Vena saphena magna or greater saphenous vein) or hollow of the knee (Vena saphena parva or small saphenous vein) is used to locate and interrupt the entry of the stem vein into the deep venous system. Subsequently, the affected vein segment can be pulled out via a probe.
Through further development of this method, the performance of the operation is very gentle and can usually be carried out on an outpatient basis. After the operation, compression stockings should be worn during the day for about three weeks.
Radiofrequency therapy (VNUS Closure Fast) of the stem veins
In this form of treatment, a catheter is placed under ultrasound control in the affected stem vein. A cut in the groin or popliteal fossa (hollow of the knee) is not necessary. Subsequently, the vein wall is heated while protecting the surrounding tissue, the vein then closes and is removed by the body. However, existing branches are not treatable with this method and are removed by crocheting or sclerosing in the same session.
The advantages of this method are the best possible cosmetic result and almost normal mobility and resilience the day after the operation. However, not every varicose vein finding is suitable for this type of treatment.
Each form of therapy involves risks, side effects, and complications. Even with the best possible care, a desired result can not be guaranteed. Therefore, a detailed explanation is provided before each intervention.
FAQ
How does the blood drain when the affected vein segments are removed?
The outflow of blood from the leg is about 90% via the deep venous system and about 10% via the superficial veins. If veins have developed into varicose veins, they lose their function, that means the blood can not be properly transported back to the heart in this area and other veins have to take over this function. Such varicose veins thus provide more harm than good and can be safely removed.
How do I behave after an operation on the varicose veins?
Running (not jogging!) is easily possible and recommended right after the surgery. Depending on the procedure, we recommend wearing compression stockings during the day and for at least a week. Showering is possible after a short time; bathing and swimming should be avoided for 2-3 weeks. Sun exposure is to be avoided for at least 4 weeks due to the risk of pigmentation disorders.
Does my health insurance fund take over radiofrequency treatment?
This form of therapy is currently not a benefit of the statutory health insurance. If a suitable finding is submitted, each patient will receive a cost estimate upon request, which can be submitted to the health insurance company for examination.